PSLD – Most Advanced Technology to Treat Back Pain with a Small Wound and Less Risk
Lumbar Spinal Stenosis
Back pain and lower back pain often cause irritation and take a toll on the body. Some sufferers may not even be able to work or go about their daily routine. The most common cause of back and lower back pain is lumbar spinal stenosis.
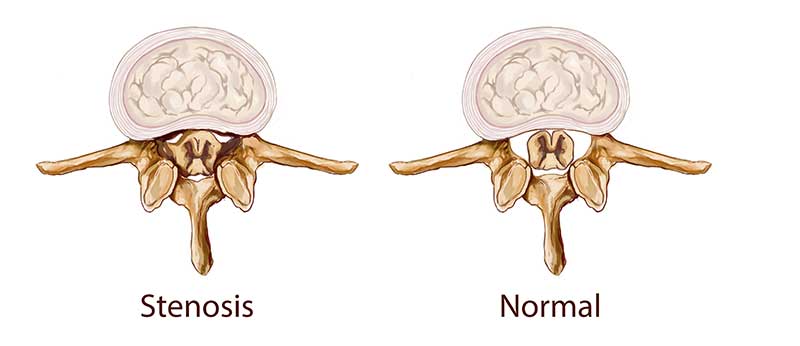
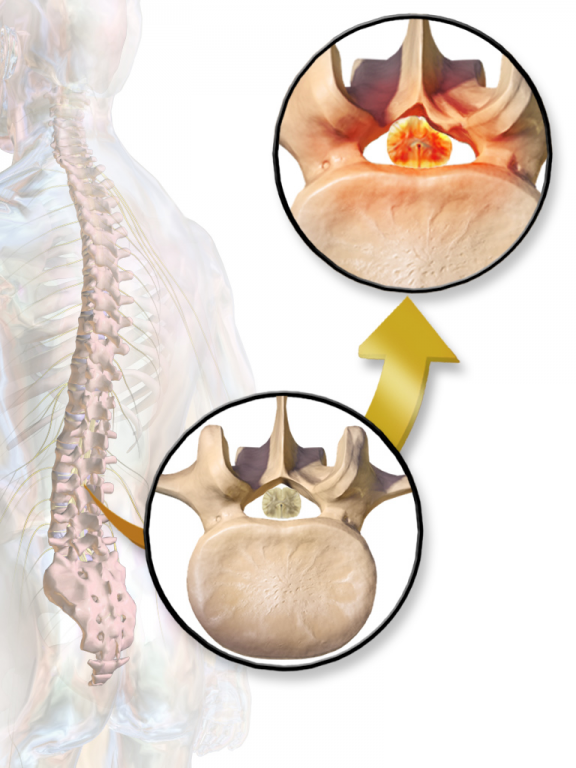 Lumbar spinal stenosis is a narrowing of the spinal canal which houses nerves of the spinal cord. The narrowing may just be in one area of the spinal cord or more areas. It could be caused by the thickening of the bone, the thickening of the tendon, dislocation of the spinal disc, spondylolisthesis, or a combination of any of these factors.
Lumbar spinal stenosis is a narrowing of the spinal canal which houses nerves of the spinal cord. The narrowing may just be in one area of the spinal cord or more areas. It could be caused by the thickening of the bone, the thickening of the tendon, dislocation of the spinal disc, spondylolisthesis, or a combination of any of these factors.
Narrowing of spinal canal
Most Common Causes
1.Defect of the spinal canal since birth
2.Degeneration of the spinal canal according to age
3.Illness or other factors such as illnesses related to the bones (osteoporosis, spondylosis)
Symptoms
Lumbar spinal stenosis causes back pain which can spread down to one leg or both legs at the same time. Patients may also feel a weakening of the leg muscle or pain in the legs and thighs which requires them to take frequent stops while walking. These are caused by pressure on the nerves or blood not flowing to the nerves. Walking will be impacted thus affecting patients’ daily living.
Moreover, patients may feel pain and numbness around the buttocks or the pelvis area and it may spread to the legs while walking or standing for a long period of time. It may also disrupt urination and bowel movement (such as not being able to hold urine, not being able to urinate, and/or constipation) and may even lead to impotency in men.
Most symptoms occur while bending over or sitting down. There are usually no symptoms and less pain when sleeping on the back or bending forward but bending backwards will cause symptoms to intensify.
When to See a Doctor
 You should see a doctor if you have leg pain (some may not experience pain in the leg); intense back pain which affects walking and daily living and causes you to have to stop a lot while walking or be able to walk shorter distances; muscle atrophy in the legs; or abnormal urination or bowel movements. You should also see a doctor if you are experiencing leg pain along with fever, weight loss, loss of appetite, or pain while lying down or during nighttime. These may indicate an infection or spinal cancer.
You should see a doctor if you have leg pain (some may not experience pain in the leg); intense back pain which affects walking and daily living and causes you to have to stop a lot while walking or be able to walk shorter distances; muscle atrophy in the legs; or abnormal urination or bowel movements. You should also see a doctor if you are experiencing leg pain along with fever, weight loss, loss of appetite, or pain while lying down or during nighttime. These may indicate an infection or spinal cancer.
Who’s Susceptible
 1. Those aged 50 or above
1. Those aged 50 or above
2. Obese people
3. Those with diabetes
4. Women who reach menopause
Diagnosis
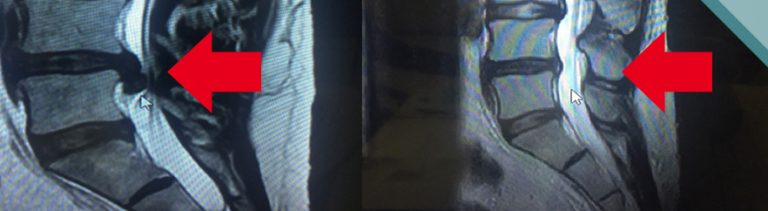
Doctors can diagnose lumbar spinal stenosis from symptoms when patients give their medical history, physical examination, x-ray, and Magnetic Resonance Imaging (MRI). The initial step is an x-ray of the spine to assess if there is any abnormality. The x-ray will help confirm the doctor’s diagnosis (results of the lower back spine x-ray will have to show signs of spinal disc spondylosis and spinal joint spondylosis). Doctors will not rely only on the x-ray results (main reliance on patient’s symptoms and physical examination) because the x-ray may show abnormalities but the patient may not have any symptoms. If the patient does not respond to treatment like they should or if there are more severe symptoms like muscle atrophy, irregular urination and bowel movement, or the patient requires surgery, the doctor may request an MRI of the spine to assess the abnormality of the spine, the spinal canal, and whether the bone is pressuring the nerve.
 Treatment
Treatment
Treatment of lumbar spinal stenosis involves medication, physical therapy, and surgery.
1. Medication includes:
-Antibiotics to lessen slight to medium pain but side effects include stomach pain, lesions in the stomach lining, and liver and kidney problems;
-Painkillers such as paracetamol to lessen pain;
-Muscle relaxants to lessen the tensing of the muscle and related pain;
-Cocktail of medicines to lessen pain and infection such as NSAIDs with muscle relaxants;
-Anti-depressants (which affect the nervous system) to lessen pain from pressure on nerves;
-Medication to prevent seizure (which affects the nervous system) to lessen pain from pressure on nerves.
2. Physical therapy to address pain such as nerve stimulation through Transcutaneous Electrical Nerve Stimulation (TENS), massage, ultrasound waves, acupuncture, traction, and strengthening the back and leg muscles to improve their efficiency.
3. Surgery becomes an option when medication and physical therapy do not work, the symptoms affect everyday living, and urination and bowel movement become uncontrollable. The objective of surgery is to lessen the pressure on the nerves and the spinal cord, to sustain the spinal cord, to remove the lamina to lessen pressure on the nerves, to remove any abnormal bone growth (in the case of abnormal bone growth), and/or to remove the fractured or degenerated spinal discs for herniated disc injuries. Surgery may utilize the fusion technique to connect bones using metal plates for patients who suffer from such severe degenerated spinal discs that the integrity of their spinal cord is compromised as well as patients who have to have their herniated discs removed affecting the strength of their spinal cord or possibly cause their spinal cord to dislocate.
 The treatments mentioned above are traditional treatments. We now have more advanced treatments which yield better results, are safer, and put less strain on the body. That is endoscopic surgery through an incision that is just 0.5 centimeters in diameter.
The treatments mentioned above are traditional treatments. We now have more advanced treatments which yield better results, are safer, and put less strain on the body. That is endoscopic surgery through an incision that is just 0.5 centimeters in diameter.
Percutaneous Stenoscopic Lumbar Decompression: PSLD
For endoscopic surgery to treat lumbar spinal stenosis, the doctor will insert the endoscopic decompression through an incision which is just 5.0 millimeters wide. The lens of the endoscopic decompression is at the end so it is as if the doctor has eyes inside the patient’s body, allowing them to see the abnormality clearly and to cut out problem areas without having to cut out muscles which are still in working condition.
 Benefits of PSLD Surgery
Benefits of PSLD Surgery
1.Small incision wound of just 0.5 centimeters in diameter
2.Less blood loss
3.Speedy recovery; patient would be able to get up after surgery
4.High level of safety
5.Low risk of infection
6.Requires just an overnight stay in hospital
7.Lower cost
8.Lessens damage to good tissue around wound
9.Immediate resumption of daily routine post-surgery
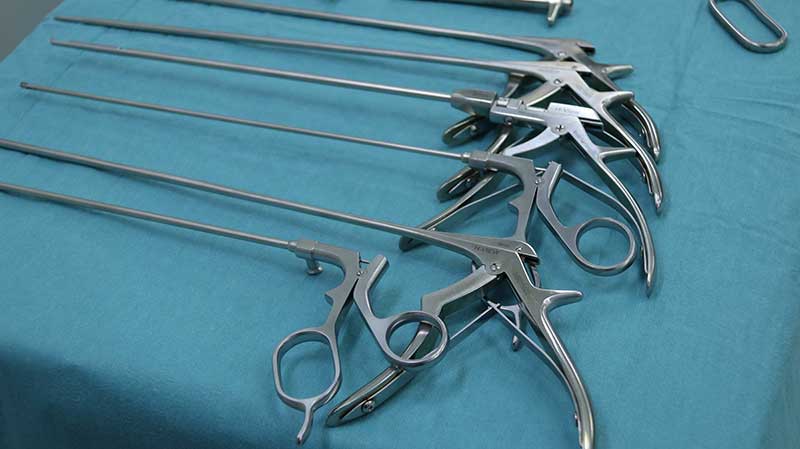 The endoscopic decompression is “a surgical instrument which is smaller than a pen.” It is a small pipe with a diameter of 5.0 millimeters and lens at one end. The edge of the lens is a little slanted for a better view of internal organs. Inside the pipe are fiber optic cables to aid in viewing as well as a small pipe to deliver water.
The endoscopic decompression is “a surgical instrument which is smaller than a pen.” It is a small pipe with a diameter of 5.0 millimeters and lens at one end. The edge of the lens is a little slanted for a better view of internal organs. Inside the pipe are fiber optic cables to aid in viewing as well as a small pipe to deliver water.
Procedure to Treat Lumbar Spinal Stenosis through PSLD
 Once the patient is under anesthesia, the doctor will insert the endoscopic decompression into the 5.0 millimeter incision to the area of the nerves which are affected. There is no need to cut out muscles in working condition. The endoscopic decompression will help the doctor see the nerves clearly and cut out parts of any herniated discs, joints, or tendons which are putting pressure on the nerves. The procedure takes about 30-45 minutes and patients will be able to get up and walk about right after surgery.
Once the patient is under anesthesia, the doctor will insert the endoscopic decompression into the 5.0 millimeter incision to the area of the nerves which are affected. There is no need to cut out muscles in working condition. The endoscopic decompression will help the doctor see the nerves clearly and cut out parts of any herniated discs, joints, or tendons which are putting pressure on the nerves. The procedure takes about 30-45 minutes and patients will be able to get up and walk about right after surgery.
Preventing Lumbar Spinal Stenosis
If you think you are at risk of developing lumbar spinal stenosis, here are steps you can take to try to prevent it from happening to you:
1.Lose weight to lessen the pressure on your spine
2.Treat and control your other chronic illnesses
3.Avoid bending over and sitting in the same posture for a long period of time
4.Adjust the way you use your back
5.Undergo physical therapy even when at home
6.Exercise daily but avoid excessive exercise









